After spontaneous rupture of membranes, this fetal heart rate pattern is observed. The initial intervention should be to:
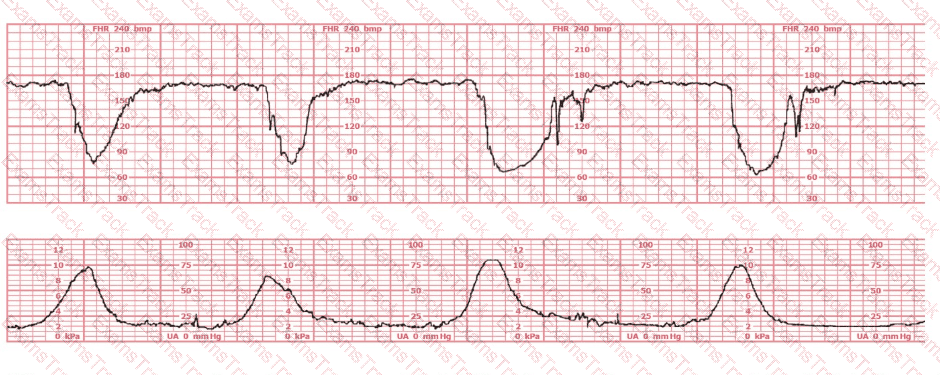
A patient presents at 38-weeks gestation with complaints of decreased fetal movement and ruptured membranes. The fetal heart rate is not able to be determined with an external ultrasound monitor. A spiral electrode is placed, and the tracing shows a rate of 90 bpm. What is the next most appropriate action?
When auscultating the fetal heart rate, the Doppler should be placed over the fetal:
A woman at 39-weeks gestation is in early labor, 2–3 cm dilated, 85% effaced, and –2 station. Based on the fetal heart rate tracing shown, what is the most appropriate first intervention?
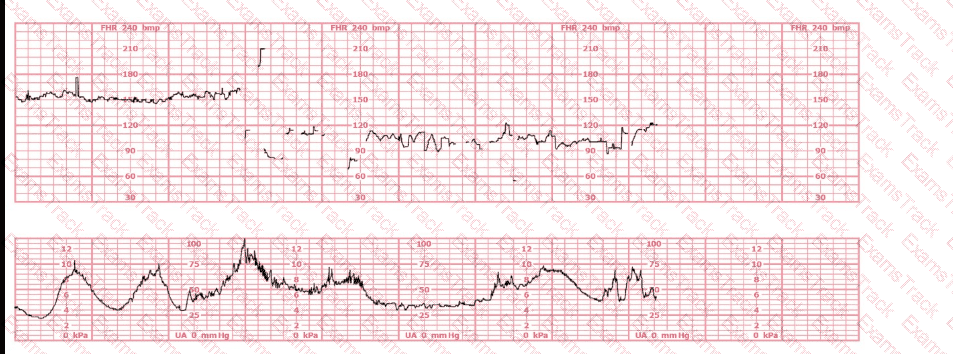
The fetal heart rate tracing shown demonstrates:
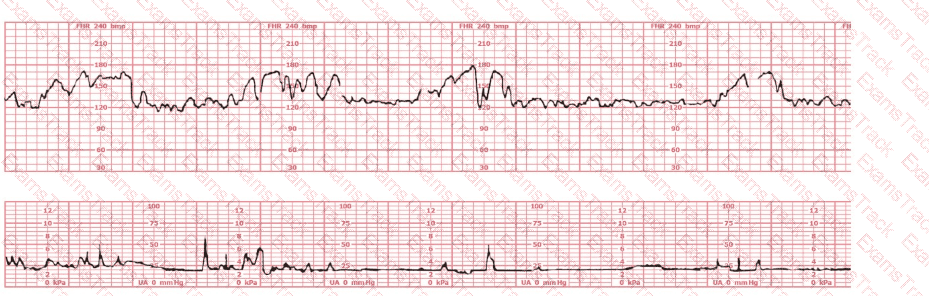
A fetal heart rate tracing is abnormal. A change in maternal position and oxygen administration do not correct the pattern. Following birth, a fetal cord blood sample is taken:
pH = 7.25
PaCO₂ = 46 mm Hg
PaO₂ = 20 mm Hg
HCO₃ = 22 mEq/L
Base deficit = –4 mEq/L
These results are best interpreted as:
Fetal respiratory acidosis is most likely to present with which of the following fetal heart rate decelerations?
This patient received an epidural 15 minutes prior to the tracing shown. The next course of action is to:
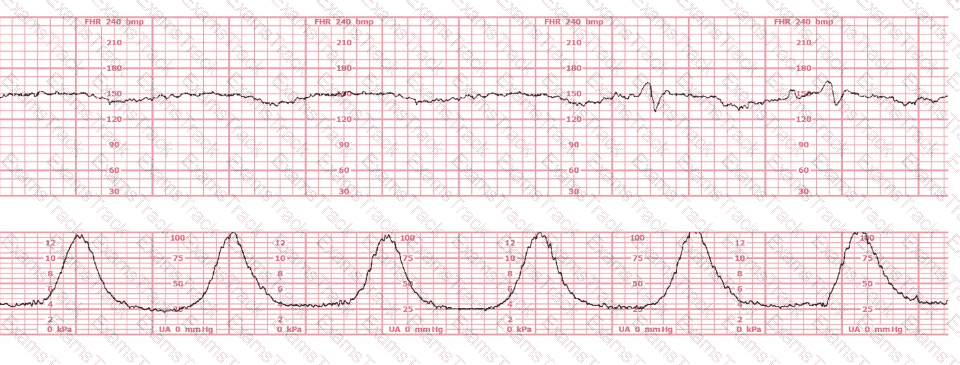
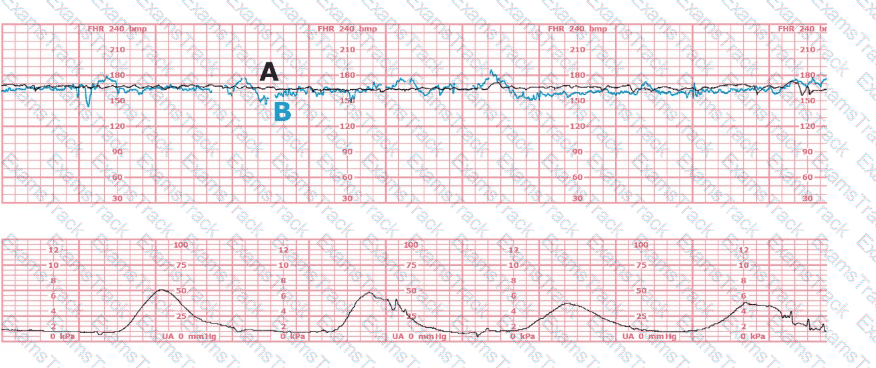
The black pattern represents the heart rate pattern for Baby A. The blue pattern represents the heart rate pattern for Baby B. A possible etiology of the baseline fetal heart rate of Baby A is:
A woman with hypertension at 38-weeks gestation has a biophysical profile. The result is 4/10 with decreased amniotic fluid volume. The next step should be to: